Introduction
Migraine is a prevalent neurological disorder characterized by recurrent moderate-to-severe headaches, accompanied by photophobia, phonophobia, nausea, and vomiting. It presents complex pathophysiology involving both central and peripheral mechanisms, including peripheral and central sensitization, lack of habituation, thalamo-cortical dysrhythmia, and hyperexcitability of the motor cortex. These mechanisms are crucial contributors to the substantial burden of migraine.1,2 According to the Global Burden of Disease (GBD) studies, migraine impacts over one billion people and is a primary cause of disability worldwide.3,4 Since 1990, the burden of migraine (encompassing absolute case counts, crude rates, and DALYs) has risen significantly. This increase is particularly pronounced in low- and middle-income countries (LMICs), where healthcare resources are often limited.5–7 The condition severely impairs quality of life and functional capacity.8 Beyond its health impact, migraine also imposes a substantial economic toll. In India, for example, productivity losses are estimated at 17.3 workdays per patient annually, amounting to approximately $22.21 billion.9 Migraine not only poses a strain on healthcare systems, such as increased resource requirements, but also diminishes individual well-being. Hence, it is imperative to address migraine in LMICs.10
Women of reproductive age (15–49 years) are disproportionately affected and represent a high-risk subgroup. Hormonal fluctuations during these years are known to exacerbate and chronify migraine.11,12 Furthermore, in many LMICs, socioeconomic factors (eg., unpaid caregiving duties) and environmental exposures (eg., PM2.5 air pollution) may further compound the risk and burden in this population.9,13 Consequently, focused attention on the disease burden among reproductive-age women in LMICs is essential.
Although GBD studies have provided valuable insights into global migraine prevalence, current global analyses remain limited for this vulnerable population, as most studies aggregate data across broad regions or general populations without targeted long-term trend assessments of migraine burden among reproductive-age women in LMICs.5,14 These gaps necessitate updated, targeted analyses. Therefore, the current research aims to comprehensively examine trends in migraine burden among reproductive-age women (15–49 years) in LMICs from 1990 to 2023. To achieve this, we analyzed recent GBD 2023 data using advanced analytical methods, including decomposition analysis and projections. The findings are expected to inform targeted prevention and control strategies for this vulnerable population.
Materials and Methods
Data Sources
The officially published GBD 2023 database was used for all analyses in the current study. GBD offers systematic estimates for 463 diseases and injuries across 204 countries and territories from 1990 to 2023. In the GBD framework, these estimates are generated by synthesizing diverse sources, including censuses, household surveys, disease registries, and scientific literature. Standardized modeling tools (eg., DisMod-MR 2.1) are then applied to ensure consistency and comparability of the estimates (Global Burden of Disease Study 2023, IHME, 2024).10,15
Migraine burden estimates for reproductive-age women (15–49 years) in LMICs were extracted from the Global Health Data Exchange results tool. These estimates comprised key metrics: prevalence, incidence, and DALYs, all of which were reported alongside 95% uncertainty intervals (95% UI). Estimates were first extracted for 5-year age strata (15–19, 20–24, 25–29, 30–34, 35–39, 40–44, 45–49 years), then directly aggregated to derive the overall reproductive-age group (15–49 years) by summing case counts and calculating population-weighted crude rates. DALYs rates were standardized per 100,000 population for cross-population and temporal comparisons.
Disease and Key Indicator Definitions
Disease Definition
Migraine was defined as per the International Classification of Headache Disorders (3rd edition) as a primary headache disorder. It is marked by recurrent, moderate-to-severe headaches. These headaches are often unilateral and pulsating, and typically accompanied by photophobia, phonophobia, or nausea.16 International Classification of Diseases (ICD) codes (ICD-9: 346–346.93 and ICD-10: G43-G43.919) were utilized to identify cases in the GBD study.15,16
GNI
Countries were stratified by economic level using the World Bank’s 2023 fiscal year classification, which is based on GNI per capita.17 GNI per capita reflects the total domestic and foreign value added claimed by a country’s residents. It is a key indicator for comparing economic development. According to this classification, the 2023 income categories are: low-income (GNI-L; ≤ $1,145), lower-middle-income (GNI-LM; $1,146–$4,515), and upper-middle-income countries (GNI-UM; $4,516–$14,005). Our analysis focused on 129 LMICs as per this classification. The following aggregated groups were created: “LMICs”, “GNI-L”, “ GNI-LM”, and “ GNI-UM”.
Socio-Demographic Index (SDI)
The SDI is a composite indicator developed by the Institute for Health Metrics and Evaluation (IHME) to quantify societal development. It integrates educational attainment among individuals aged 15 and older, average lag-distributed income per capita, and the total fertility rate under 25.18
Statistical Analysis
Estimated Annual Percentage Change (EAPC) and Percentage Change
To quantify the temporal trends in migraine burden among reproductive-age women (15–49 years) in LMICs from 1990 to 2023, two key metrics were employed: the EAPC and the percentage change.16

The 95% confidence interval (CI) for the EAPC was calculated using a linear regression model.19 The trend was interpreted as follows. Where both the EAPC value and the lower bound of its 95% CI exceeded 0, a significant increasing trend was identified. Where both the EAPC and the upper CI bound were below 0, the trend was considered significantly decreasing. In cases where the 95% CI included 0, no statistically significant trend was concluded.20
Percentage change was used to assess the overall relative change in the absolute number of cases (eg., prevalent cases, incident cases) or the crude rate between the start year (1990) and the end year (2023). It was calculated as:
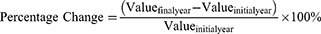
This measure provides a straightforward interpretation of the total magnitude of change over the entire study period and complements the annualized trend captured by the EAPC.15
Decomposition Analysis
To elucidate the respective contributions of demographic transitions and epidemiological transformations to the trends in migraine burden among reproductive-age women (15–49 years) in LMICs from 1990 to 2023, a decomposition analysis was performed using the Das Gupta method.14,16 This approach quantitatively disaggregates total changes in disease burden metrics—such as incidence, prevalence, and DALYs—into components attributable to three key factors: population growth, population aging, and epidemiological changes. The contributions of these three components were calculated as absolute differences and relative percentages of the total observed change. A positive contribution indicated that the factor increased the disease burden over the period, whereas a negative contribution signified that the factor reduced the burden.14 This analysis provided critical insights into the underlying drivers of migraine burden trends and informed targeted public health interventions.
Autoregressive Integrated Moving Average (ARIMA) Model
The ARIMA model was applied to forecast the future trends in migraine burden, specifically DALYs, among reproductive-age women (15–49 years) in LMICs up to the year 2050.10,21 The ARIMA framework is a potent statistical technique for time series analysis and prediction. It effectively captures underlying patterns, trends, and potential seasonal fluctuations. The ARIMA (p, d, q) model integrates three key components: the autoregressive (AR) component (p), the differencing (I) component (d), and the moving average (MA) component (q). Historical data on annual DALYs from 1990 to 2023 were used as the training dataset for model fitting. The optimal combination of (p, d, q) parameters was determined using a systematic approach. The approach minimized information criteria, specifically the Bayesian information criterion (BIC) and Akaike information criterion (AIC). Therefore, it ensured a parsimonious and well-fitting model.15 The fitted ARIMA model was then used to generate projections for DALYs (with 95% uncertainty intervals [UIs]) from 2024 to 2050. This provided a probabilistic assessment of future burden trends.
This study was conducted in accordance with the Declaration of Helsinki. Since the research involved the secondary analysis of publicly available, de-identified data from GBD, it was exempted from formal ethical review by the Institutional Review Board of PKUCare Rehabilitation Hospital. This exemption is based on Items 1 and 2 of Article 32 of the “Measures for Ethical Review of Life Science and Medical Research Involving Human Subjects” (issued on February 18, 2023, by the National Health Commission of China), which stipulate that ethical review may be exempted for research utilizing publicly available data or anonymized data. Informed consent was not required as the data were aggregated and did not contain identifiable personal information.15,22 The results were reported following the Strengthening the Reporting of Observational Studies in Epidemiology guidelines.23
Statistical analyses were conducted in R (v4.3.2). Significance was defined as a two-sided p-value < 0.05.
Results
Trend Analysis
LMICs
From 1990 to 2023, the absolute burden (absolute numbers of prevalent cases, incident cases, and DALYs) of migraine increased substantially among women aged 15–49 years in LMICs. The most notable elevation was observed in DALYs (68%, 95% UI: 62–74%), followed by prevalent cases (67%, 95% UI: 61–73%) and incident cases (61%, 95% UI: 55–67%) (Table S1). As this study focused on a narrow reproductive-age population and did not conduct age standardization, the crude rates were examined and exhibited an upward trend, with the most pronounced increase seen in DALYs (EAPC: 0.17, 95% UI: 0.16–0.18).
In addition, Joinpoint regression analysis was implemented to delineate the temporal trajectory and identify potential inflection points. The results confirmed a consistent, significant upward trend from 1990 to 2023. The average annual percentage changes (AAPCs) were 0.33% for DALYs, 0.31% for prevalence, and 0.10% for incidence (P < 0.05 for all). However, the temporal patterns diverged among the three metrics (Figure 1). The prevalence stabilized around the year 2000 and then increased. The incidence exhibited a more volatile trajectory, with multiple phases of expansion and contraction. It had three distinct expansion phases: 1990–1995 (APC = 0.06), 2000–2005 (APC = 0.23, P < 0.05), and 2013–2020 (APC = 0.17). Such expansion was interrupted by two contraction periods: 1995–2000 (APC = −0.17, P < 0.05) and 2005–2013 (APC = −0.07). Conversely, DALYs increased steadily after 1996.
GNI
The EAPCs further highlighted divergent trends across income groups. Significant declines were observed in GNI-L and GNI-LM, while notable increases were seen in GNI-UM (EAPCs for GNI-UM: 0.31 for prevalence, 0.09 for incidence, and 0.34 for DALYs; Table S1). Joinpoint analysis elucidated this divergence by revealing distinct temporal trajectories. Sustained declines were observed in GNI-L across all indicators throughout the study period. The steepest reductions in prevalence occurred during 2012–2017, and the steepest reductions in incidence occurred during 2012–2018. A more modest overall reduction in the disease burden was noted in GNI-LM; however, this trend was interrupted by a transient increase in DALYs between 2010 and 2015. Conversely, the most significant increase was seen in GNI-UM. The elevation was marked by sharp rises in prevalence and DALYs between 2015 and 2019.
National Level
At the national level, the most substantial percentage increases in migraine burden were observed in Jordan, Equatorial Guinea, and Djibouti. This heterogeneity aligned with the SDI-based findings. For instance, the disease burdens in Peru (with the most marked deterioration in age-standardized DALYs, EAPC = 0.41) and China (EAPC = 0.39) exceeded SDI-based expectations. A similar pattern was observed for prevalence and/or DALYs in Brazil, Thailand, Iran, and Egypt. A contrasting divergence was observed in incidence, which was lower than expected in Peru, Djibouti, and Rwanda but higher in the Philippines, Iran, and Indonesia (Table S2–S7, Figures 2 and 3).
Analysis of the Correlation Between the SDI and GNI
A detailed correlation analysis at the national level further clarified the intricate relationship between economic development and migraine burden. No statistically significant linear correlations were observed between GNI per capita and any indicator for migraine burden (P > 0.05) (Figure 4). However, substantial heterogeneity was observed when examining the SDI. Analysis of the observed-to-expected ratios across SDI quintiles revealed marked divergence in burden levels by country (Figure 5). The prevalence was notably lower than expected in countries such as Ethiopia and Malawi and notably higher than expected in Brazil and Thailand. A similar pattern was noted for DALYs: lower-than-expected prevalence values were seen in Ethiopia and Mozambique, while higher-than-expected prevalence values were identified in Iran and Egypt. The incidence was lower than expected in South Sudan and Rwanda, and higher than expected in Iran and Indonesia. Overall, these data revealed substantial heterogeneity in migraine burden across countries with similar levels of development. The results highlighted the influence of unique contextual factors beyond aggregate socioeconomic indicators.
Age-Specific Trends
Across LMICs, migraine incidence peaked among women aged 25–29 and then gradually declined with age. In contrast, both prevalence and DALYs increased with age, peaking at 40–44 years of age and then decreasing slightly. The highest rates were consistent across all age groups in GNI-L (Figure 6).
Decomposition Analysis
Decomposition analysis revealed distinct drivers of the increasing migraine burden among women aged 15–49 across income subgroups in LMICs (Figure 7 and Table S8). From 1990 to 2023, prevalence, incidence, and DALYs increased consistently across all GNI subgroups. The most pronounced elevation was in GNI-LM, followed by GNI-L and GNI-UM. Population growth was the dominant driver. Notably, population expansion contributed 107.18% to the increase in prevalent cases in GNI-L (exceeding the total observed increase, with other components partially offsetting burden growth), 100.59% in GNI-LM, and 53.62% in GNI-UM. This illustrated its varying influence across different levels of socioeconomic development.
In contrast, epidemiological changes offset 1.58% to 8.06% of the effect of population expansion in GNI-L and GNI-LM. However, these changes contributed 37.24% to 45.42% to the increase in GNI-UM.
Population aging had a modest, though varied, influence on migraine burden. The direction of its effect (exacerbating or protective) depended on the specific measure and country income level.
ARIMA Model
An ARIMA model was fitted to the 1990–2023 DALYs series for women aged 15–49 in GNI-L and GNI-LM. The model was then used to project the burden to 2050. The optimal model orders, together with the corresponding AIC, BIC, and Ljung–Box test p-values, are reported in Table S9. The Ljung–Box statistic indicated white-noise residuals for the chosen model parameters (p > 0.05). This confirmed an adequate model fit and stability.
Unlike the global downward trajectory reported for several other neurological disorders, the projected DALYs for migraine in this population increased modestly but steadily over the next 26 years. Specifically, the model estimates that age-standardized DALYs will rise from 954.42 (95% CI: 943.81–965.03) per 100,000 individuals in 2024 to 994.98 (95% CI: 980.66–1,009.30) per 100,000 individuals by 2050. This represents an average annual increment of 1.56 per 100,000 individuals (Figure 8). The projections are provided in Table S10.
Discussion
The present research used the GBD 2023 data to comprehensively analyze the trends of migraine burden from 1990 to 2023 among reproductive-age women (15–49 years) in GNI-L and GNI-LM. Our findings revealed a significant upward trajectory in migraine burden. The overall increase was approximately 67% in prevalent cases, 61% in incident cases, and 68% in DALYs over the 33-year period. Differences in burden drivers were observed across economic subgroups. Population growth was the dominant factor in GNI-L and GNI-LM. In GNI-UM, epidemiological changes acted in concert with demographic factors to significantly exacerbate the burden. Given this key distinction, stratified public health responses are required. Additionally, the ARIMA model projects a continued rise in DALYs, which are expected to reach 994.98 per 100,000 by 2050. This further underscores that targeted interventions are necessary.15,16
The current analysis first quantified a substantial increase in the absolute burden (absolute case numbers) of migraine among women aged 15–49 in LMICs from 1990 to 2023. Significant upward trends were also noted in crude rates. This confirmed that the burden of migraine intensified beyond what demographic changes alone would predict. This rising burden is driven by population growth and aging, suggesting that healthcare systems in these countries may face mounting pressure in the coming years.15 The Joinpoint analysis further refined the understanding of these temporal patterns. The results revealed that the steady rise in prevalence and DALYs masked a more volatile trajectory of incidence, marked by distinct expansion and contraction phases. This volatility suggests that incident cases of migraine may be more sensitive to transient societal, environmental, or diagnostic factors than the more cumulative indicators of prevalent cases and DALYs.
Stratified analysis was performed by income level. The results revealed a sustained decline in the disease burden in GNI-L and a pronounced surge, particularly after 2015, in GNI-UM. This finding is different from the traditional review of a uniformly increasing burden across LMICs. The steepest reductions in GNI-L and the sharp increases in GNI-UM demonstrate that the stage of economic development is a pivotal determinant of migraine burden trajectory. This divergence is strongly supported by the opposing EAPCs across these income subgroups.
The correlation analysis further elucidated the complex relationship between economics and disease burden. The absence of significant linear correlations between GNI per capita and burden metrics suggests that wealth alone does not directly predict migraine burden. The variations in migraine burden were observed across countries at different levels of development. This pattern may be partly explained by increasing exposure to environmental and occupational risk factors during economic transition. Simultaneously, the necessary healthcare infrastructure and public awareness for effective migraine management often lag behind during this period.24,25
Additionally, the substantial heterogeneity observed within SDI quintiles and at the national level underscores the limitations of aggregate economic and developmental indices. Specifically, Brazil, Thailand, and Iran consistently exhibited a higher-than-expected burden. Ethiopia, Malawi, and Mozambique showed a lower-than-expected burden. This discrepancy points to the powerful influence of unique national contexts. Contextual factors, such as specific healthcare policies, environmental regulations, and cultural attitudes, are crucial for comprehending and addressing the migraine burden at an actionable, country-specific level.16,18
The observed age-specific patterns revealed a distinct biphasic burden profile, requiring life-course intervention. The peak of incidence in the 25–29 age group likely reflects a convergence of early-career stressors, maximal hormonal volatility associated with the peak reproductive years, and systemic barriers to healthcare access when initiating childbearing.11,12,26 In contrast, the peak of prevalence and DALYs shifted to the 40–44 age group. This change highlights the cumulative effects of disease chronicity and significant work-family strain, which often hinders effective self-management. Furthermore, it underscores the impact of earlier perimenopausal onset commonly observed in these populations. These factors contribute to accumulating disability over time.6,27 Additionally, crude migraine rates were consistently highest across all age groups in GNI-L, highlighting an amplified, non-age-specific vulnerability. Such a vulnerability can be attributed to a constellation of factors prevalent in resource-limited settings, including pervasive diagnostic delays, limited access to preventive and acute treatments, and potentially greater exposure to environmental triggers. This confluence of challenges culminates in a higher overall burden, regardless of the specific life stage.6
The decomposition analysis provides critical, detailed insights into the divergent drivers of the increasing migraine burden across economic subgroups. It moves beyond describing overall trends to identify and quantify the underlying drivers.14,16 The findings confirm that the substantial increase in the absolute burden masks fundamentally different underlying mechanisms when stratified by income. In GNI-L and GNI-LM, population growth accounted for more than 100% of the observed net increase across all metrics, overwhelmingly and consistently driving the rise. In these settings, epidemiological changes (as reflected in age-specific rates) paradoxically exerted a slight protective effect, offsetting some of the growth driven by demographics. This pattern strongly suggests the presence of significant diagnostic gaps and systematic underreporting in the most resource-limited settings, which may mask the true scale of the disease burden.16,24,28 Conversely, a complex tripartite driver profile was noted in GNI-UM. While population growth remained a primary contributor, its relative role was diminished. More critically, epidemiological changes acted as powerful synergistic drivers, contributing between 37.24% and 45.42% to the increase. This shift indicates that factors beyond demography are actively exacerbating the migraine burden in these economies. These likely include improved case detection, facilitated by greater healthcare access and awareness. Concurrently, increased exposure to environmental and occupational triggers—especially fine particulate matter (PM2.5) derived from rapid industrialization and urbanization in GNI-UM—exerts a critical effect. PM2.5 can induce neurovascular inflammation, oxidative stress, and meningeal vasodilation, which are core pathophysiological mechanisms of migraine. In addition, reproductive-age women with inherent hormonal fluctuations are more susceptible to such environmental exposures, further exacerbating the onset, severity, and chronicity of migraine.13,24 Furthermore, population aging has become a significant additional driver in GNI-UM, substantially increasing the burden for prevalence and DALYs. This trend reflects both the cumulative nature of the disorder and, as societies develop, a demographic shift toward a larger proportion of women within the older, higher-risk subgroups of the 15–49 age range.
The ARIMA modeling demonstrated a robust fit to the historical data and projects a concerning and persistent rise in the migraine burden among reproductive-age women in LMICs through 2050. This projected upward trend in age-standardized DALYs rates contrasts sharply with the global trajectories of several other neurological disorders. The contrast underscores migraine’s status as a growing yet uniquely neglected public health priority in these regions.10,21 This projection directly follows from the key drivers identified in our study. Without effective, targeted interventions, the relentless demographic momentum in lower-income nations and the powerful synergistic effect of epidemiological changes in GNI-UM will continue to drive the burden higher. Consequently, millions of additional DALYs are projected by 2050, with profound implications for individual well-being, healthcare systems, and economic productivity.9
The decomposition, economic correlation, and age-stratified analyses reveal that a proactive, stratified public health response is necessary to counter this projected trajectory. Therefore, a dual-pronged strategic framework is proposed. In GNI-L/LM, where population growth is the dominant driver, priorities should center on foundational strengthening. This includes scaling up community-based screening to address diagnostic delays,29 task-shifting headache care to mid-level providers to expand access,9 and ensuring the reliable availability of essential migraine medications through centralized procurement to prevent stockouts.30,31 For GNI-UM, where epidemiological changes and aging are key drivers, the focus must shift to mitigating these specific risks. This includes implementing stricter environmental regulations on PM2.5 emissions,21 integrating subsidized neuromodulation devices and newer prophylactics such as CGRP inhibitors into public health coverage systems,9,32 and leveraging AI-assisted platforms to reduce diagnostic delays.33 Across all subgroups, legislative models ensuring migraine-friendly workplaces are crucial to reducing productivity losses and the resultant employment disadvantages.30,34 Hence, implementing these income-sensitive and age-aware strategies is imperative to alter the current trajectory and mitigate the rising burden of migraines among reproductive-age women in LMICs.
The present investigation has several inherent limitations. First, diagnostic constraints and significant resource limitations, particularly in Sub-Saharan Africa, likely lead to an underestimation of the true disease burden.6 Second, while GBD modeling provides standardized estimates, its reliance on extrapolation in regions with limited surveillance data may introduce geographic bias. Differences in case identification methods across income groups also contribute to methodological heterogeneity.35,36 Third, because current migraine disability weights do not fully capture cognitive impairment or the interictal burden, they may underestimate the full impact of the disease.8,21 Finally, the inherent time lag in GBD 2023 data means that the analysis may not fully reflect recent disruptions in healthcare delivery. While the ARIMA projections are statistically robust, they cannot incorporate the effects of unforeseen therapeutic advances or health policy reforms.15
Conclusion
Our analysis reveals a substantial increase in the absolute burden of migraine (crude rates and absolute case numbers) among women aged 15–49 years in LMICs from 1990 to 2023. The absolute number of incident cases, prevalent cases, and DALYs elevated substantially by 67%, 61%, and 68%, respectively. This surge was predominantly driven by population growth, which contributed over 100% of the net increase in GNI-L and GNI-LM. Notably, the subgroup analysis by income revealed different drivers. Epidemiological factors exerted a slight protective effect in lower-income settings, but acted as a significant synergistic driver in GNI-UM, contributing 37%–45%. Additionally, population aging differentially influenced disease metrics across income levels.
These findings underscore the imperative to develop income-stratified public health strategies. The results are generalizable to reproductive-age women (15–49 years) with migraine in LMICs, providing robust evidence for the monitoring of population-level burden and targeted interventions. For other populations (eg., males, postmenopausal women, or individuals in high-income countries), the burden trends and driving mechanisms may differ due to hormonal variations, socioeconomic disparities, and divergent healthcare conditions. In clinical practice, the data support risk screening and tailored management for reproductive-age women. In public health policy, they provide a reference for the allocation of resources and preventive planning across LMICs at different economic levels. In lower-income regions, strategies should focus on foundational strengthening of healthcare systems to manage the demographic-driven burden, including community-based screening and task-sharing initiatives. In contrast, GNI-UM must prioritize mitigating epidemiological risks through environmental regulations and by integrating advanced therapies into healthcare systems. For achieving UN Sustainable Development Goal 3, it is necessary to integrate migraine management into primary healthcare frameworks. Specific attention should be paid to the divergent burden patterns identified in this study.
Data Sharing Statement
The original contributions presented in the study are included in the article; further inquiries can be directed to the corresponding author.
Author Contributions
All authors contributed significantly to the reported work, whether in its conception, study design, execution, data acquisition, analysis, or interpretation; participated in drafting, revising, or critically reviewing the article; gave final approval of the version to be published; agreed on the journal to which the article was submitted; and agreed to be accountable for all aspects of the work.
Funding
The authors declare that they did not receive any funding from any source.
Disclosure
The authors declare that they have no competing interests in this work.
References
1. Deodato M, Granato A, Martini M, Sabot R, Buoite Stella A, Manganotti P. Instrumental assessment of pressure pain threshold over trigeminal and extra-trigeminal area in people with episodic and chronic migraine: a cross-sectional observational study. Neurol Sci. 2024;45(8):3923–16. doi:10.1007/s10072-024-07372-4
2. Su M, Yu S. Chronic migraine: a process of dysmodulation and sensitization. Mol Pain. 2018;14:1744806918767697. doi:10.1177/1744806918767697
3. Terruzzi A, AlMadani A, Al-Rukn S, et al. A retrospective analysis of disease epidemiology, comorbidity burden, treatment patterns, and healthcare resource utilization of migraine in the United Arab Emirates. Pain Ther. 2024;13(5):1235–1255. doi:10.1007/s40122-024-00634-1
4. Korolainen MA, Tuominen S, Kurki S, et al. Burden of migraine in Finland: multimorbidity and phenotypic disease networks in occupational healthcare. J Headache Pain. 2020;21(1):8. doi:10.1186/s10194-020-1077-x
5. Takizawa T, Danno D, Ishii R, et al. The dual impact of ictal and interictal burden in migraine: an analysis from the ObserVational survey of the Epidemiology, tReatment, and Care Of MigrainE (OVERCOME) Japan second study. J Headache Pain. 2025;26(1):140. doi:10.1186/s10194-025-02079-z
6. Aderinto N, Olatunji G, Kokori E, et al. Prevalence, characteristics, and treatment outcomes of migraine headache in Nigeria: a systematic review and meta-analysis. J Headache Pain. 2024;25(1):172. doi:10.1186/s10194-024-01869-1
7. Satapathy P, Chauhan S, Gaidhane S, et al. Trends in migraine and tension-type headaches in South Asia: findings from the Global Burden of Disease Study 2021 (1990-2021). Front Neurol. 2025;16:1514712. doi:10.3389/fneur.2025.1514712
8. Lo SH, Gallop K, Smith T, et al. Real-World experience of interictal burden and treatment in migraine: a qualitative interview study. J Headache Pain. 2022;23(1):65. doi:10.1186/s10194-022-01429-5
9. Saha S, Chowdhury D, Wadhwa M, et al. Impact of migraine on productivity and efficiency among adult population in India: a scoping review. J Headache Pain. 2025;26(1):180. doi:10.1186/s10194-025-02112-1
10. Steinmetz JD, Seeher KM, Schiess N, et al. Global, regional, and national burden of disorders affecting the nervous system, 1990-2021: a systematic analysis for the Global Burden of Disease Study 2021. Lancet Neurol. 2024;23(4):344–381. doi:10.1016/S1474-4422(24)00038-3
11. Ansari T, Lagman-Bartolome AM, Monsour D, Lay C. Management of menstrual migraine. Curr Neurol Neurosci Rep. 2020;20(10):45. doi:10.1007/s11910-020-01067-x
12. Cupini LM, Corbelli I, Sarchelli P. Menstrual migraine: what it is and does it matter? J Neurol. 2021;268(7):2355–2363. doi:10.1007/s00415-020-09726-2
13. Portt AE, Orchard C, Chen H, Ge E, Lay C, Smith PM. Migraine and air pollution: a systematic review. Headache. 2023;63(9):1203–1219. doi:10.1111/head.14632
14. Qin C, Liu M, Liu J. Trends and disparities of disease burden in infections among pregnant women in 131 low-income and middle-income countries, 1990-2019. J Glob Health. 2024;14:04130. doi:10.7189/jogh.14.04130
15. Wang YX, Lu GS, Zhao JJ, et al. The burden of migraine and predictions in the Asia-Pacific region, 1990-2021: a comparative analysis of China, South Korea, Japan, and Australia. J Headache Pain. 2025;26(1):104. doi:10.1186/s10194-025-02048-6
16. Cen J, Wang Q, Cheng L, Gao Q, Wang H, Sun F. Global, regional, and national burden and trends of migraine among women of childbearing age from 1990 to 2021: insights from the Global Burden of Disease Study 2021. J Headache Pain. 2024;25(1):96. doi:10.1186/s10194-024-01798-z
17. Bank TW. World bank country and lending groups. https://datahelpdesk.worldbank.org/knowledgebase/articles/906519. Accessed October 08, 2025.
18. Wijeratne T, Oh J, Kim S, et al. Global, regional, and national burden of headache disorders, 1990-2021, with forecasts to 2050: a Global Burden of Disease study 2021. Cell Rep Med. 2025;6(10):102348. doi:10.1016/j.xcrm.2025.102348
19. Yu Q, Xue F, Wik SL, et al. Mapping disease burden of major depressive disorder and its risk factors in low- and middle-income countries. Psychother Psychosom;2025. 1–11. doi:10.1159/000547927
20. Hua Y, Liu J, Ji K, Han W. Global trends and regional disparities in atrial fibrillation and flutter burden attributable to high alcohol consumption: findings from the global burden of disease study 2021. BMC Cardiovasc Disord. 2025;25(1):266. doi:10.1186/s12872-025-04699-4
21. Dong L, Dong W, Jin Y, Jiang Y, Li Z, Yu D. The global burden of migraine: a 30-year trend review and future projections by age, sex, country, and region. Pain Ther. 2025;14(1):297–315. doi:10.1007/s40122-024-00690-7
22. Piccininni M, Brinks R, Rohmann JL, Kurth T. Estimation of migraine prevalence considering active and inactive states across different age groups. J Headache Pain. 2023;24(1):83. doi:10.1186/s10194-023-01624-y
23. Della Pietra A, Gómez Dabó L, Mikulenka P, et al. Mechanosensitive receptors in migraine: a systematic review. J Headache Pain. 2024;25(1):6. doi:10.1186/s10194-023-01710-1
24. Stovner LJ, Hagen K, Linde M, Steiner TJ. The global prevalence of headache: an update, with analysis of the influences of methodological factors on prevalence estimates. J Headache Pain. 2022;23(1):34. doi:10.1186/s10194-022-01402-2
25. Kang S, Eum S, Chang Y, et al. Burden of neurological diseases in Asia from 1990 to 2019: a systematic analysis using the Global Burden of Disease Study data. BMJ Open. 2022;12(9):e059548. doi:10.1136/bmjopen-2021-059548
26. Alwhaibi M, Alhawassi TM. Humanistic and economic burden of depression and anxiety among adults with migraine: a systematic review. Depress Anxiety. 2020;37(11):1146–1159. doi:10.1002/da.23063
27. Wei D, Wong LP, He X, Loganathan T. Healthcare utilisation and economic burden of migraines among bank employees in China: a probabilistic modelling study. J Headache Pain. 2024;25(1):60. doi:10.1186/s10194-024-01763-w
28. Duburcq A, Molins M, Debremaeker S, et al. Overview of migraine care, impact of the disease, and patient experience in France through patient voices: a cross-sectional and participatory survey study. J Headache Pain. 2025;26(1):76. doi:10.1186/s10194-025-02018-y
29. Zhao Y, Yi Y, Zhou H, Pang Q, Wang J. The burden of migraine and tension-type headache in Asia from 1990 to 2021. J Headache Pain. 2025;26(1):49. doi:10.1186/s10194-025-01990-9
30. Lin L, Zhu M, Qiu J, et al. Spatiotemporal distribution of migraine in China: analyses based on baidu index. BMC Public Health. 2023;23(1):1958. doi:10.1186/s12889-023-16909-9
31. Zhang YJ, Li XY, Guo ZL. Temporal trends of migraine and tension-type headache burden across the BRICS: implications from the Global Burden of Disease study 2019. Front Neurol. 2023;14:1307413. doi:10.3389/fneur.2023.1307413
32. Barbanti P, Aurilia C, Torelli P, et al. Three-year treatment with anti-CGRP monoclonal antibodies modifies migraine course: the prospective, multicenter I-GRAINE study. J Neurol. 2025;272(2):170. doi:10.1007/s00415-025-12911-w
33. Sun X, Chen B, Qi Y, et al. Multi-omics Mendelian randomization integrating GWAS, eQTL and pQTL data revealed GSTM4 as a potential drug target for migraine. J Headache Pain. 2024;25(1):117. doi:10.1186/s10194-024-01828-w
34. Getz M, Charleston L, Armand CE, Willis AW, Seng E. Perceived discrimination and migraine-specific quality of life: a cross-sectional survey study in a Black/African American sample. Headache. 2025;65(10):1839–1849. doi:10.1111/head.14970
35. Wang L, Qin X, Jin L, et al. Global, regional, and national burden of atrial fibrillation and flutter associated with metabolic risk factors, 1990-2021. Front Cardiovasc Med. 2025;12:1578908. doi:10.3389/fcvm.2025.1578908
36. Huang K, Huang X, Qian S, Cai Y, Wu F, Luo D. Temporal trends of thyroid cancer in China and globally from 1990 to 2021: an analysis of the global burden of Disease Study 2021. Sci Rep. 2024;14(1):25538. doi:10.1038/s41598-024-77663-5








