
Civil Society, Featured, Global, Global Governance, Headlines, Health, IPS UN: Inside the Glasshouse, Population, Poverty & SDGs, TerraViva United Nations
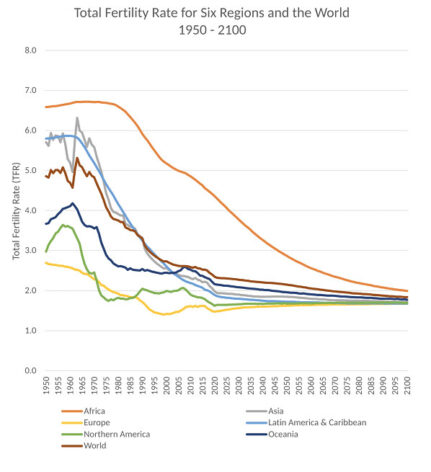
Total Fertility Rate (TFR) is the average number of children that would be born to a woman over her lifetime. Source: World Population Prospects 2022 report from the Population Division of the United Nations Department of Economic and Social Affairs
– As birthrates continue to decline in many industrialized countries, anxious governments are running out of schemes to keep women procreating.
In the US, millionaires and billionaires are lining up to donate to Trump’s “baby bonus” savings accounts. Trump accounts give parents $1,000 for all babies born between now and 2028, plus whatever private donors add.
Late last year tech billionaires Michael and Susan Dell donated $6.25 billion to them. The accounts are part of Trump’s far-Right pronatalist agenda, and also part of the broader trend of governments using heavy-handed pronatalist policies, ranging from bribes to outright coercion, to convince women to have more babies and shore up the supply of future workers, taxpayers, and soldiers.
These interventions are notoriously ineffective. A recent Heritage Foundation report recommended using economic incentives to convince American women to have more babies, “with preferences for larger-than-average [families],” while shaming those who choose to have fewer or no children.

A family in South Korea, which has the lowest Total Fertility Rate in the world (0.8).
But it also admitted, “Other nations have tried to reverse declining birthrates through financially generous family policies, none has succeeded. Government spending alone does not ensure demographic success.”
Nor can such policies achieve what Heritage calls “success.” Trying to raise birthrates by incentivizing women to have babies not only undermines hard-won reproductive rights, it’s a waste of money.
Such spending is not a priority for U.S. taxpayers, as most Americans do not see falling birth rates as a crisis. Instead, they overwhelmingly want the government to address untenably high child care costs. But a one-time Trump account infusion makes no dent in high costs of raising children and other barriers to motherhood.
Just as recent cuts to SNAP and Medicaid disproportionately affect marginalized women and children, Trump accounts benefit least those who need help most. By the Administration’s own calculations, the accounts will benefit wealthy parents disproportionately.
This shouldn’t be surprising. Trump accounts and other pronatalist policies aren’t really about empowerment or saving families or supporting children. They are a bid to make more white Americans, part of a larger nativist program which includes cracking down on immigration from African and Muslim countries, detaining and deporting non-white people in huge numbers, and even abandoning former U.S. efforts to fight child exploitation and trafficking.
These policies overtly stoke panic about falling birthrates, and tacitly uphold the white supremacist “great replacement” conspiracy theory.
That makes support for pronatalism from some progressives especially disturbing. Even if their intent is not nativist, advocating policies that push women to have more children is anti-feminist and fundamentally at odds with reproductive agency.
And even when such policies intend to serve feminist goals–for example Finland’s generous parental leave and child and health care—they fail to raise birthrates. That’s because the biggest factor in childbearing decisions isn’t affordability; it’s empowerment.
Nobel prizewinning economic historian Claudia Goldin has shown high birthrates are no longer tied to economic prosperity, as women increasingly choose education and careers over traditional family roles. In fact, she found an inverse relationship between per capita income and fertility. “Wherever you get increased agency,” she said, “you get reduction in the birth rate.”
Another study across 136 countries confirms this: whenever women achieve reproductive agency, birthrates decline, whether the economy is growing or shrinking.
But hundreds of millions of women and girls are denied this agency. Over 640 million alive today were child brides (including in the US). Over 220 million have an unmet need for contraception. More than half of pregnancies are unintended—121 million annually. Cuts in USAID and other aid programs make the situation more dire.
Despite birthrates declining in many countries, global population is going up, projected to swell by 2 billion to 10.4 billion by the 2080s, with vast ecological and social consequences. Extreme climate events are expected to kill more than a billion people and displace up to 3 billion this century, most in countries where women and girls are disempowered and fertility rates remain high. Pronatalism will only make ecological and social crises worse.
We need new policy thinking that recognizes this and embraces the many advantages of declining fertility and less growth. As fertility rates fall, female labor participation will increase and gender pay gaps will narrow.
As median age rises, changing demographics could enable policy shifts that improve wages and conditions for workers and extend job opportunity to billions on the sidelines who want work but don’t have it.
There is no lack of good ideas, from economic models that center wellbeing and rethink growth to radical ecological democracy. Exploring them requires getting off the endless growth treadmill that enriches elites at the expense of the rest of us. We must stop treating women like reproductive vessels for making more people to serve the economy, and start reshaping our economies to serve more people and the planet.
Nandita Bajaj is executive director of the NGO Population Balance, senior lecturer at Antioch University, and producer and host of the podcasts OVERSHOOT and Beyond Pronatalism. Her research and advocacy work focuses on addressing the combined impacts of pronatalism and human expansionism on reproductive and ecological justice.
IPS UN Bureau












